Arthroscopic Surgery
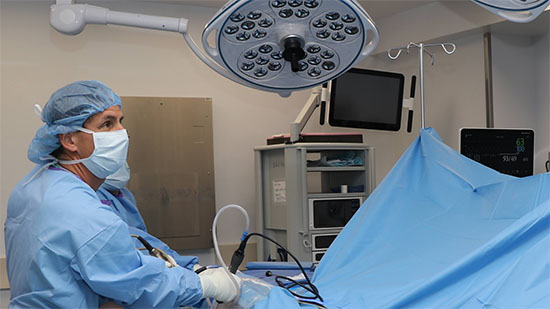
Arthroscopic surgery is a procedure that allows surgeons to directly view the inside of a joint in order to diagnose and treat numerous orthopedic conditions. During the procedure, the surgeon creates a “portal” or small incision to introduce an arthroscope, a pencil-sized fiber-optic camera, into the joint, which magnifies and transmits the image to a high-definition television monitor. Additional portals are created to introduce specially designed instruments into the joint to remove or repair diseased or injured tissues.
Arthroscopic surgery is performed in an operating room under general, regional or local anesthesia. As it is minimally invasive, patients can typically go home the same day (outpatient or ambulatory surgery) and require little or no pain medication afterward.
Dr. L’Insalata is board certified in Orthopaedic Surgery and subspecialty certified in Orthopaedic Sports Medicine and specializes in arthroscopic surgery of the knee and shoulder.
Ligament & Tendon Repair/Reconstruction
Ligaments are strong bands of connective tissue that connect the ends of bones to one another, providing stability and support for our joints. Tendons are the fibrous cords that connect our muscles to bone. Ligament injuries (“sprains”) and tendon injuries (“strains”) are the most common orthopedic injuries. Most ligament and tendon injuries can be treated non-surgically with an initial RICE protocol (Rest, Ice, Compression, and Elevation) followed by a home exercise regimen or physical therapy and sometimes bracing or immobilization to protect the injured area. Some complete tears of ligaments and tendons are best managed with surgical repair or reconstruction in order to restore full function.
Common ligament injuries include those of the ankle, knee, shoulder, wrist and hand. Common tendon injuries include those of the shoulder (rotator cuff, biceps), elbow (biceps, triceps, lateral extensor), knee (patella and quadriceps tendons), and ankle (Achilles, posterior tibial).
Dr. L’Insalata commonly performs arthroscopic and open repair and reconstruction of ligaments and tendons when conservative care alone is unable to satisfactorily restore their function.
Rotator Cuff tears
 The Rotator Cuff are a group of four muscles that join as tendons to create a “cuff” or cover over the head of the humerus at the shoulder. The rotator cuff functions to elevate and rotate your arm. The rotator cuff tendons can be injured acutely from a fall or abrupt lifting of a heavy object. More commonly, tears occur over time from wear and tear. In most patients, nonsurgical treatment including medication and physical therapy will relieve the pain and restore the function of the shoulder. If your pain and function do not improve, a rotator cuff repair surgery may be offered.
The Rotator Cuff are a group of four muscles that join as tendons to create a “cuff” or cover over the head of the humerus at the shoulder. The rotator cuff functions to elevate and rotate your arm. The rotator cuff tendons can be injured acutely from a fall or abrupt lifting of a heavy object. More commonly, tears occur over time from wear and tear. In most patients, nonsurgical treatment including medication and physical therapy will relieve the pain and restore the function of the shoulder. If your pain and function do not improve, a rotator cuff repair surgery may be offered.
Dr. L’Insalata commonly performs rotator cuff repair surgery arthroscopically and via “mini-open” or minimally invasive techniques in an outpatient or ambulatory setting.
Glenoid Labrum tears, SLAP tears, Biceps Surgery
The glenoid labrum is a soft fibrous tissue (fibrocartilage) that surrounds the socket (glenoid) of the shoulder joint to improve the stability of the joint. The labrum is also the attachment site of the important glenohumeral ligaments. The glenoid labrum and associated ligaments are most commonly injured from an acute trauma such as a fall onto an outstretched arm but can also be damaged from repetitive overhead activities such as in baseball, tennis and weightlifting. Glenoid labrum tears commonly occur following shoulder dislocations.
The long head of the biceps also runs within the shoulder joint to attach to the superior aspect of the glenoid labrum. The labrum can tear at the biceps anchor causing a Superior Labrum Anterior and Posterior (SLAP) tear. These tears can occur from similar mechanisms to glenoid labrum tears as well as from motor vehicle accidents and forceful overhead jerking of the arm.
In most cases, nonsurgical treatment including rest and physical therapy are sufficient in relieving symptoms and restoring normal shoulder function following glenoid labrum and SLAP tears. In some cases, symptoms persist despite proper conservative care and surgery may be offered. This typically consists of arthroscopic labral repair and/or SLAP repair in which sutures are placed to repair the damaged tissue via small arthroscopic incisions or portals. In certain circumstances, an open reconstruction may be indicated to best restore the shoulder function. Certain SLAP tears, particularly those with associated damage to the biceps tendon, are best managed with a biceps tenotomy (release of biceps at its attachment) or biceps tenodesis in which the long head of the biceps is removed from inside the shoulder joint and reattached outside the joint.
Dr. L’Insalata routinely performs arthroscopic glenoid labrum repair, arthroscopic SLAP repair and biceps tenodesis in an outpatient ambulatory setting.
Meniscus tears (Arthroscopic meniscectomy & meniscus repair)
The knee menisci are C-shaped, fibrous disks that act as shock absorbers of the knee. Meniscus tears can occur from a single acute injury, particularly those involving a twisting mechanism. They can also occur from “wear and tear” over time, often referred to as a “degenerative tear.” Meniscus tears often cause pain and swelling in the knee and can sometimes cause catching or locking.
Many tears, particularly degenerative tears, can improve with nonsurgical treatment including rest, anti-inflammatory medication, and therapeutic exercises. If symptoms persist with non-surgical treatment, arthroscopic surgery can be performed to repair the meniscus or to trim the torn, unstable portion of the meniscus (meniscectomy). The ability to repair the meniscus depends upon the pattern and location of the tear which affects the blood supply to the meniscus and impacts its ability to properly heal. Meniscal repair is performed arthroscopically, placing sutures and small implants into the meniscus to align and fix the tear. Repairing the meniscus may reduce the potential to develop arthritis following a meniscal tear. The goal is to repair any meniscal tear when appropriate. Tears that are not amenable to repair are treated with partial meniscectomy.
Dr. L’Insalata routinely performs outpatient arthroscopic meniscal surgery with general, spinal or local anaesthesia. He will thoroughly discuss treatment options based upon your individual condition including associated injuries, activity level, age, goals, physical examination and x-ray or MRI findings.
ACL tears, Arthroscopic ACL reconstruction
The anterior cruciate ligament (ACL) runs diagonally in the middle of your knee, connecting the femur (thigh bone) to the tibia (leg bone). It prevents the tibia from sliding out in front of the femur. The ACL typically tears from a forceful twisting or hyperextension injury to the knee as occurs with an abrupt change of direction or pivot with the foot planted on the ground or from a direct impact injury such as in a football tackle.
The evaluation and diagnosis of an ACL tear is made by a combination of a thorough clinical history and physical examination and diagnostic testing including x-rays and MRI. Treatment of ACL tears will vary based upon associated injuries and depending on the patient’s individual needs. In less active patients and those with sufficient overall stability, non-surgical methods may be recommended. This will typically involve activity modification, physical therapy and sometimes bracing. Younger athletes involved in pivoting sports will likely require surgery to safely return to playing.
The usual surgery for an ACL tear is an arthroscopic ACL reconstruction in which your surgeon will replace the torn ligament with a local tissue graft from yourself (autograft) or a donor graft (allograft). Dr. L’Insalata will speak with you to help you to choose the best treatment including graft type for you. Rehabilitation will be needed following surgery to help restore the normal range of motion, strength and overall function of the knee.
Sports Medicine
Sports Medicine is a field of medicine that deals with physical fitness and the prevention and treatment of injuries and disorders related to participation in sports and exercise. Sports Medicine specialists may include doctors from the fields of medicine, family practice or orthopaedic surgery who have often completed further training such as a Sports Medicine fellowship. Sports injuries can occur while playing sports or exercising and can result from accidents, inadequate training, insufficient warm-up exercises, or improper use of protective devices. The most common sports injuries are sprains, strains, fractures, and dislocations.
Dr. L’Insalata is a board certified orthopaedic surgeon who completed a fellowship in Sports Medicine at the University of Pittsburgh Medical Center and regularly treats sports related injuries. Dr. L’Insalata has received a Subspecialty Certificate in Orthopaedic Sports Medicine from the American Board of Orthopaedic Surgery, awarded to Board-Certified orthopaedic surgeons who have demonstrated qualifications in sports medicine beyond those expected of other orthopaedic surgeons by virtue of additional training, a practice characterized by a volume of cases in sports medicine, or have made significant contributions to the field of Sports Medicine.
Fracture Care
A fracture is a broken bone. Fractures most commonly are caused by a trauma such as a fall, sports injury, or motor vehicle accident. Fractures can also occur from repetitive overuse leading to a stress fracture or in association with a weakened bone due to a bone tumor or to osteoporosis, a disorder leading to generalized weakening of the bones. A suspected fracture is evaluated and diagnosed by a combination of clinical history, physical examination, and radiographic imaging such as x-rays and sometimes CT scan or MRI.
Fracture treatment depends on many variabilities including the specific bone injured, the fracture severity, pattern and location, bone quality, associated injuries, and patient-specific variables including age, activity level, and overall health. Most fractures will naturally heal on their own and the goal of treatment is to optimize the speed of healing and the function of the bone and joints following healing while minimizing any potential complications.
Fracture treatment generally involves aligning the bones to allow restoration of function, immobilizing and protecting the fractured area, and therapeutic exercises to maintain and restore function. For many fractures this can often be performed in an office setting with the use of casts, splints, braces or slings while some fractures are best managed surgically. Surgery allows for fracture reduction (realignment) and internal fixation / immobilization of the fracture with the use of plates and screws or pins, intramedullary nails, or external fixators. Some severe fractures as best managed with surgical replacement of the injured bone using a prosthesis such as a hip or shoulder replacement. Your doctor will fully assess your injury and make recommendations as to which form of treatment would be best for you.
Arthritis Treatment, Hyaluronic Acid and Platelet-Rich Plasma (PRP) injections
Arthritis is degeneration or inflammation of one or more joints. It typically causes pain and stiffness in the joint and sometimes swelling. Arthritis may be categorized as degenerative (osteoarthritis), posttraumatic, inflammatory (rheumatoid, lupus, gout, Lyme, psoriatic) or septic (infection). Treatment of arthritis will vary depending upon the exact cause and the severity of symptoms.
While there is no cure for arthritis, treatment can help relieve the pain and disability it can cause. Treatment may include activity modification, therapeutic exercises, and sometimes a brace or assistance device such as a cane or walker to reduce stress on the joint. Oral medications such as acetaminophen (Tylenol) or nonsteroidal anti-inflammatory medications (ibuprofen, naproxen) can help relieve pain.
Joint injections with cortisone can help reduce pain and inflammation while viscosupplementation (hyaluronic acid, “gel” injection) can help in joint lubrication and relief of osteoarthritis pain. Platelet–rich plasma (PRP) is obtained from your own blood after it has been processed to concentrate platelets and growth factors that can enhance healing and reduce inflammation. PRP can be injected into damaged tissues or joints in the office. PRP is currently considered investigational so is often not covered by insurance.
For more advanced arthritis that is non-responsive to conservative measures, surgery may be indicated. This may include arthroscopic surgery or more commonly joint replacement arthroplasty. After a complete evaluation, Dr. L’Insalata can help you choose the best treatment regimen.
Carpal Tunnel Surgery
Carpal tunnel syndrome is caused by compression of the median nerve at the wrist as it travels within the carpal canal. It typically causes pain, numbness and tingling in the hand. Diagnosis is usually made by a thorough history and physical examination by your physician but may also include x-rays or electrodiagnostic testing including electromyogram and nerve conduction velocity testing.
The initial treatment of carpal tunnel syndrome is usually non-surgical including wrist bracing, nonsteroidal anti-inflammatory medication, activity modification, therapeutic exercises or physical therapy and sometimes a steroid (cortisone) injection directly into the carpal canal. If non-surgical treatment does not relieve the symptoms or if the symptoms are more severe, surgery consisting of a carpal tunnel release may be recommended. The surgery consists of releasing the transverse carpal ligament (roof of the carpal canal), typically performed under local anesthesia in an outpatient / ambulatory setting.
Occupational Health/Work Injuries
Workplace injuries occur in 2 to 3 workers per 100 full-time workers and can account for significant disability and lost time from work. The most common workplace injuries include sprains, strains, and tears. Dr. L'Insalata can assess your work related injury and help devise a treatment regimen to resolve or improve your condition.
Dr. L’Insalata can also work with you to suggest work modifications which may allow you to resume work with the goal of allowing you to safely and comfortably return to your regular occupation.
